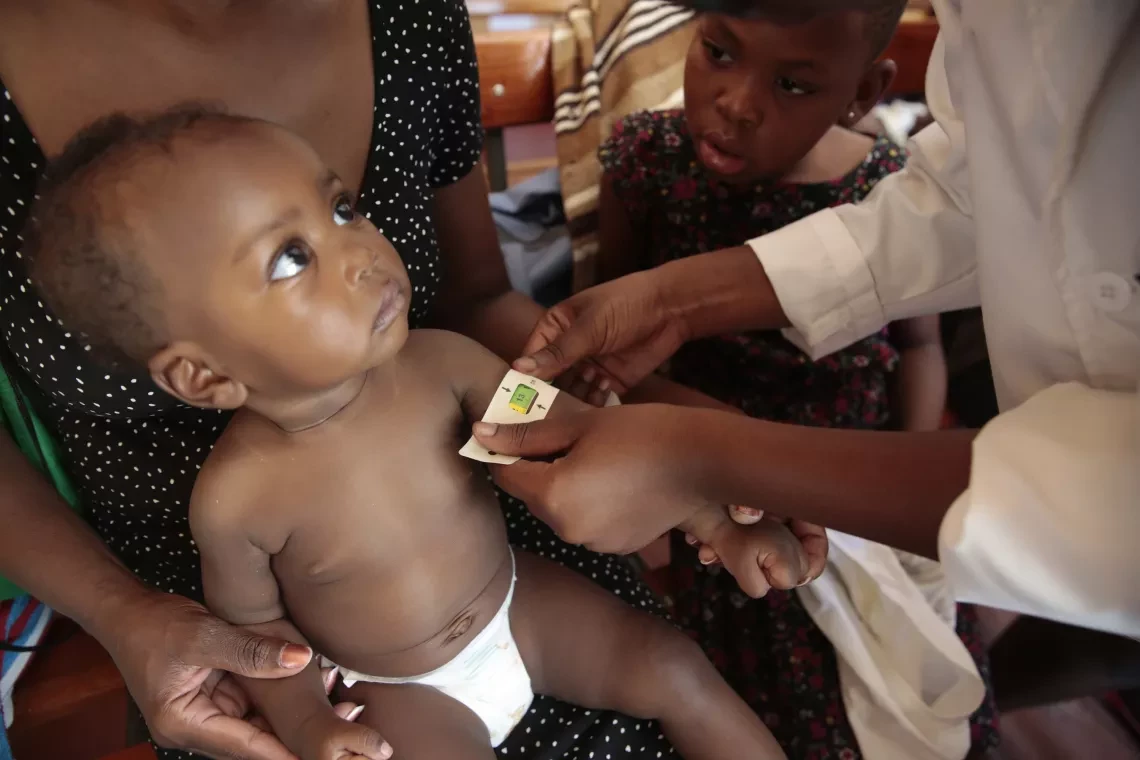
UNICEF Zimbabwe has issued an urgent appeal for US$36,5 million to respond to the pressing needs of children and families in 38 high-priority districts.
The appeal is aimed at providing lifesaving, multisectoral interventions in health, nutrition, water, sanitation and hygiene, education, child protection, and social protection.
It also integrates crucial support for HIV response, risk communication and community engagement and gender-based violence prevention.
Despite such urgent needs, Zimbabwe continues to fall short in meeting its commitment to adequately fund the health sector.
In 2001, African Union (AU) member States signed the Abuja Declaration, pledging to allocate at least 15% of national budgets to health.
The commitment was meant to strengthen fragile health systems and improve health outcomes across the continent.
Zimbabwe has struggled to meet this benchmark.
In 2022, Finance minister Mthuli Ncube allocated 14,9% of the national budget to health.
- Another ETF lists on ZSE
- Econet to use Buddie Beatz app to grow local music
- Edutainment mix: The artist in the child policy formulation context
- An unsung HIV/Aids hero spreads message of hope
Keep Reading
Since then, allocations have steadily declined: 10,5% in 2023, 10,84% in 2024, and just 10,2% in 2025.
This is far below the Abuja target and the steady decline has weakened public health delivery at a time when the needs of the population are growing exponentially.
The health sector in Zimbabwe remains heavily underfunded and donor-dependent.
According to health financing assessments, nearly 70% of health expenditure in recent years has been met through out-of-pocket payments and external partner funding, placing a heavy burden on ordinary citizens.
Many essential services — including HIV and Aids treatment, maternal and child health programmes, and vaccination campaigns — rely almost entirely on foreign aid.
However, donor support has become increasingly uncertain.
Early this year, the United States government, under an executive order issued by President Donald Trump, drastically cut foreign aid funding, which directly affected Zimbabwe’s health sector.
This reduction, combined with global funding shifts, has left major health programmes under strain.
For example, Zimbabwe’s response to HIV and Aids, tuberculosis, and malaria has for a long time been dependent on the Global Fund, while Gavi has financed a greater part of the country’s immunisation programmes.
Any disruptions to these flows put millions at risk.
Meanwhile, domestic challenges such as currency instability, inflation and competing budgetary needs have further squeezed the sector.
Health workers continue to demand better wages and working conditions, hospitals face chronic shortages of drugs and equipment, and rural communities remain underserved.
Out-of-pocket health spending by households is estimated at between 25% and 30% of total health financing, making access to healthcare a significant financial burden for the poor.
The consequences of the underfunding are reflected in the country’s health outcomes:
- Life expectancy in Zimbabwe stands at around 62 years, below the global average of 73 years.
- Maternal mortality remains high, with 363 deaths per 100 000 live births, one of the highest in southern Africa.
- Infant mortality is approximately 38 deaths per 1 000 live births and under-five mortality is about 56 per 1 000 live births, reflecting gaps in child health services.
- Malnutrition continues to affect children, with 26,2% stunted growth reported among the under fives.
Zimbabwe carries one of the world’s heaviest HIV and Aids burdens, with a prevalence rate of 11,5% among adults (15-49 years).
While progress has been made with ART coverage, sustaining the gains requires consistent financing.
The country also faces growing risks from cholera, malaria, and climate-linked health crises, which strain an already fragile system.
The underfunding of the health sector threatens progress made on child mortality rate, maternal health, disease prevention, and epidemic preparedness.
With rising humanitarian needs, climate-linked outbreaks, and dwindling donor support, there is an urgent need for the government to increase domestic investment in the health sector.
Meeting the 15% Abuja threshold is not just a continental obligation, it also a lifeline for millions of Zimbabweans whose health wellbeing depends on a functional health delivery system.






